Carole Falletta, MS, MA, PMHNP-BC, FNP-BC, RNC-EFM, IBCLC, LCCE Carole is a nurse practitioner with over 30 years of experience in nursing, specializing in women's health, newborn care, and reproductive and postpartum mental health. Actively practicing in healthcare, she supports women and families during the perinatal journey through compassionate, evidence-based care. A dual board-certified nurse practitioner in psychiatric and family health, Carole is also an International Board-Certified Lactation Consultant (IBCLC) and Lamaze Certified Childbirth Educator, combining her clinical expertise and passion for education to empower mothers and support babies.
Walk into a modern labor and delivery room and you might think you’ve stepped into a mini medical command center. Beeping monitors, IV pumps, oxygen tanks, blood pressure cuffs, and sometimes even robotic tools are all part of today’s childbirth landscape. As a nurse practitioner and childbirth educator, I get questions all the time from expectant parents: Do we really need all these machines? Are they helping—or getting in the way?
Inspired by a recent New York Times article that raised the same question, I wanted to share my perspective from inside the birth room.
The Tools We Trust—But Sometimes Question
Technology in childbirth is often used with good intentions: to monitor the baby’s heart rate, to track contractions, to administer medications like Pitocin, to offer timely pain relief, or to help safely deliver a baby in distress with tools like vacuums or forceps.
But while these devices can be life-saving when needed, they also shape how birth unfolds—sometimes in ways that aren’t always necessary or helpful.
For example:
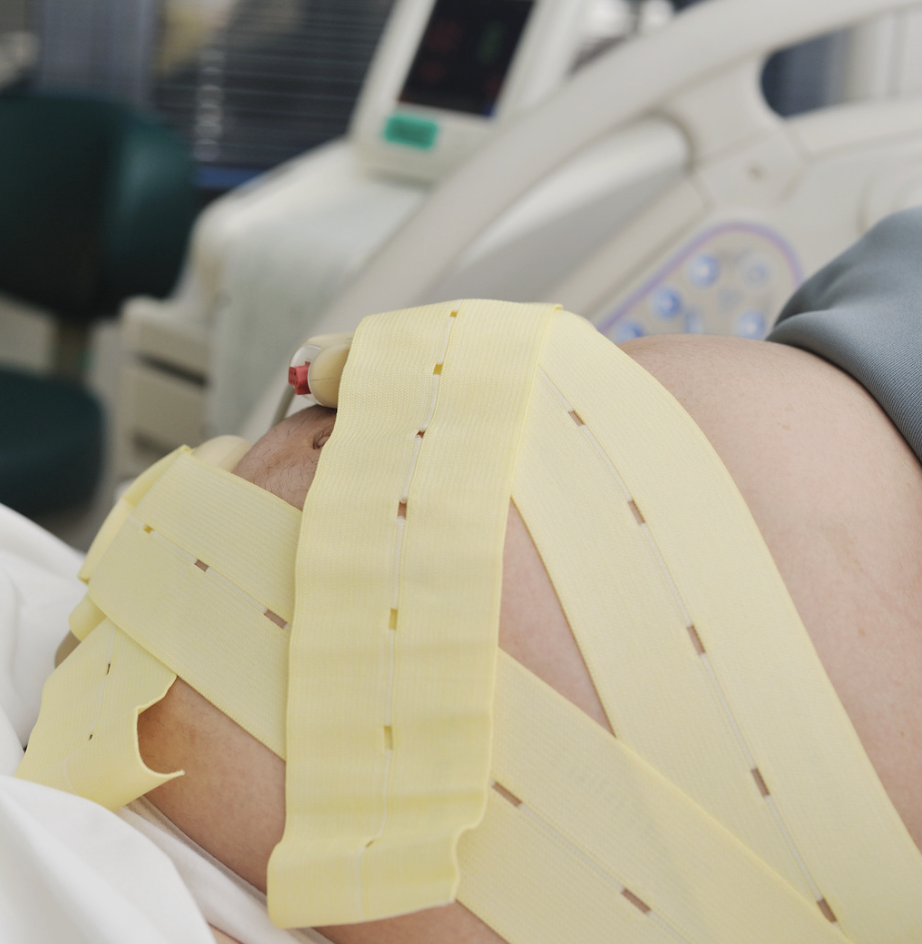
- Continuous fetal monitoring sounds reassuring, but studies show that in many low-risk pregnancies, it doesn’t improve outcomes over intermittent monitoring—and it can increase the chances of unnecessary interventions.
- IVs and automatic fluid drips can make people feel like patients instead of participants, especially when mobility becomes limited.
- Vacuum-assisted delivery can be crucial in an emergency but also has risks if not carefully weighed.

Birth Is Not a Machine
Birth is a dynamic, unfolding process. It doesn’t follow a timer, a graph, or a textbook. Sometimes when labor slows or takes a detour, our first reaction is to “fix” it with a device or a medication. But more often than not, labor just needs time, patience, position changes, hydration, and emotional support.
It’s easy to feel like something is “wrong” when a monitor beeps or a machine spits out numbers. But let’s not forget—technology should serve birth, not define it.
So, What’s the Answer?
This isn’t an anti-tech rant. It’s about balance. Many devices are incredibly helpful—especially in high-risk situations or when things aren’t going as planned. But we have to ask ourselves: Are we using this because it’s necessary, or because it’s routine?
If you’re expecting a baby, here are a few things you can do:
- Ask questions: “What is this for?” “Is it necessary right now?” “Are there alternatives?”
- Know your rights: You have a say in how you’re monitored, what procedures are used, and how you move during labor.
- Choose a provider and setting that aligns with your birth values.
- Take a quality childbirth class so you feel informed, not intimidated.
Let’s Keep the Human in the Room
No device can replace the power of eye contact, a calm voice, a supportive hand, or a care provider who listens. I’ve seen parents feel empowered and respected when their preferences were honored—and I’ve seen the opposite, when machines took center stage.
Technology belongs in the birth room. But so does trust, communication, and the deep knowing that birth is not something to be controlled—but supported.

Carole Falletta, MS, MA, PMHNP-BC, FNP-BC, RNC-EFM, IBCLC, LCCE Carole is a nurse practitioner with over 30 years of experience in nursing, specializing in women's health, newborn care, and reproductive and postpartum mental health. Actively practicing in healthcare, she supports women and families during the perinatal journey through compassionate, evidence-based care. A dual board-certified nurse practitioner in psychiatric and family health, Carole is also an International Board-Certified Lactation Consultant (IBCLC) and Lamaze Certified Childbirth Educator, combining her clinical expertise and passion for education to empower mothers and support babies.